Opinion: Regulators aren’t the main reason for your spiking energy bills
The officials who oversee Pepco don’t have control over a majority of the increases in your bill, writes Public Service Commission Chairman Emile C. Thompson.
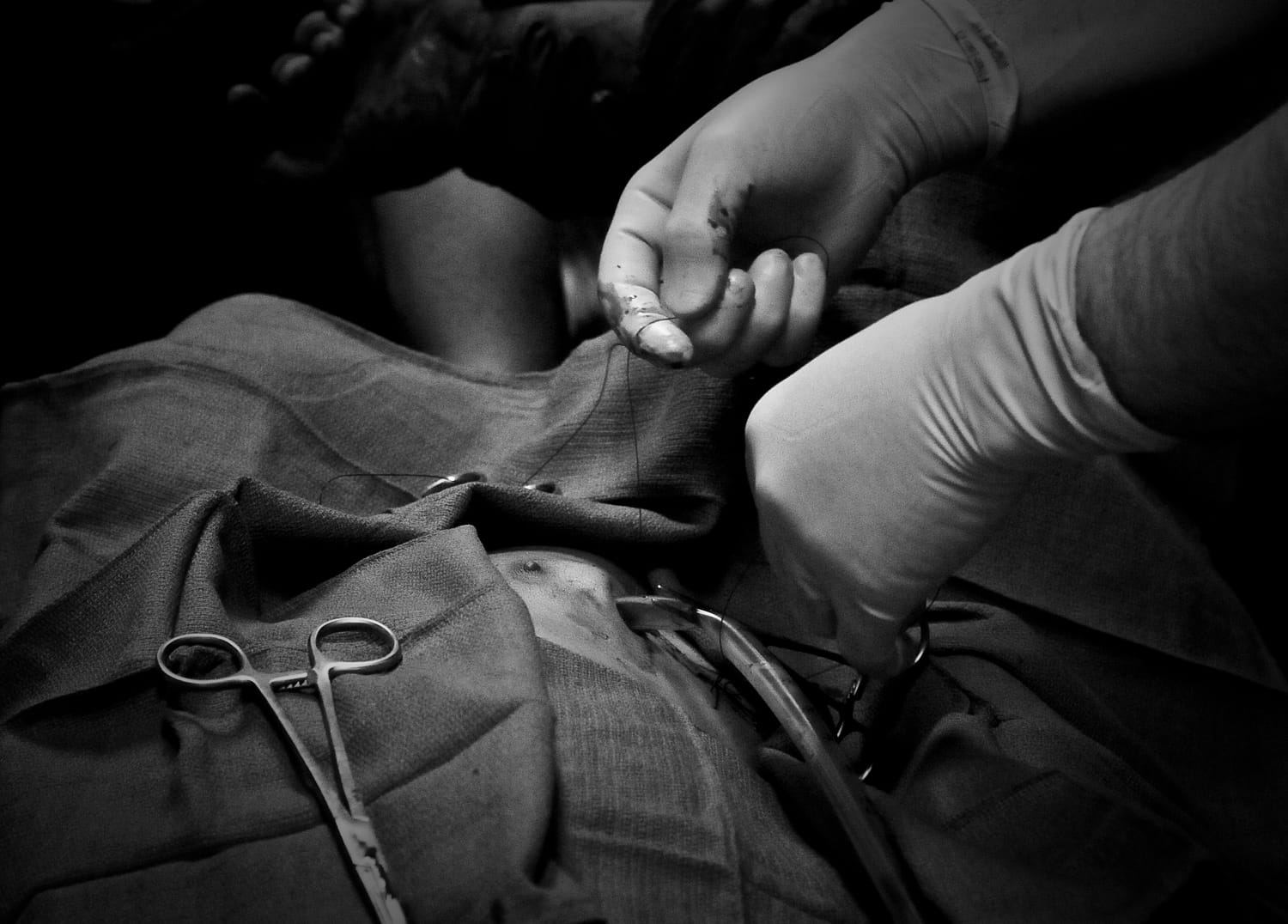
Steep city budget reductions mean patients are going without medicine, losing teeth, and living with pain.

This story was reported with support from SpotlightDC: Capital City Fund for Investigative Journalism.
Karen Hernandez has been in worse health since October.
The Ward 1 resident and mother of three has multiple conditions that require medical care. Until recently, she says she was receiving injections every six months to help with her chronic back pain, while undergoing physical therapy in preparation for surgery on her arm. That all used to be free for Hernandez through the DC Health Care Alliance, a locally funded insurance program for low-income immigrants who don’t qualify for Medicaid or Medicare.
But it all changed on Oct. 1, when the Department of Health Care Finance (DHCF) reduced Alliance members’ benefits and made it more difficult to access many forms of care. That’s in addition to implementing tighter income requirements as part of a plan to end adult enrollment on that insurance program by October 2027 — a proposal that would leave the vast majority of around 19,000 beneficiaries like Hernandez with few, if any, affordable health insurance options.
Alliance no longer covers physical therapy for adults, while injections and surgical procedures require a doctor to call for a “prior authorization,” according to the most recent member handbook. When Hernandez went to her appointments after the change, however, she says she was told her insurance no longer covers any of these services, and that another injection alone would cost her $7,000 out-of-pocket — several times the amount that her household earns in a typical month.
It all means living with more pain.
“If I walk, I feel a cramp. I feel hurt,” Hernandez told The 51st. “Sometimes I can’t walk, because it hurts.” In total, the changes mean that over 40,000 low-income D.C. residents like Hernandez have lost some of their benefits or lost their coverage entirely, according to estimates from DHCF and D.C.’s Health Benefit Exchange Authority.
At a breakfast meeting with D.C. Council members last month, Mayor Muriel Bowser characterized the recent cuts to healthcare spending as a way to address rising costs during dire financial times. She presented even bigger potential reductions — including dropping the Alliance income limit to just 24% of the federal poverty level on Oct. 1 of this year, completely eliminating adult enrollment on Alliance next year, and canceling Medicaid coverage for around 93,000 childless adults in fiscal year 2029 — as a difficult but necessary money-saving strategy as the District seeks to close a funding gap of $1.1 billion going into the next fiscal year.
“These changes are going to make these programs more sustainable for more people, for a longer period of time,” said Bowser, who declined to comment on any follow-up questions about her statements or her budget proposal until after it is introduced (it is expected in early April).
DHCF estimates that healthcare rollbacks will save about $189 million in fiscal year 2026 and $233 million in fiscal year 2027. Most of this year’s savings — about $109 million — is from Alliance changes, while $80 million comes from DHCF reducing the income limit for Medicaid.
Patients, healthcare workers, and service coordinators, however, described a heavy human toll, with some patients enduring worse health outcomes because they’re missing medicines and treatments that their insurance no longer covers. They say others are passing up work opportunities in order to meet stricter income limits, getting teeth pulled that they could have saved if they had dental insurance, or facing greater challenges finding transportation to crucial medical appointments.
Another major blow to D.C.’s healthcare programs came on Jan. 1, when DHCF cut Medicaid coverage for about 17,000 people. Most of these beneficiaries transferred to a new program, Healthy DC (also known as the Basic Health Plan), which lacks benefits like dental and vision insurance. Unlike Medicaid, this program is fully federally funded.
While the transition went smoothly from an operations perspective, many beneficiaries didn’t realize their plans had changed — leaving some care centers overwhelmed with patients who didn’t know how to access their new health plan.
Despite extensive outreach efforts both before and after the change, Mila Kofman, executive director of D.C.’s Health Benefit Exchange Authority, said she believes many people still don’t know they lost Medicaid coverage and probably won’t learn about it until the next time they try to get care.
In some cases, the consequences of this confusion might be relatively minor, just requiring a care provider to call an insurance company to get a patient’s new ID number. But other instances may be more serious. For example, Kofman said she has had limited success in contacting about 2,200 residents who lost Medicaid and don’t qualify for Healthy DC — meaning they’ll have to begin paying monthly premiums through D.C.’s Affordable Care Act marketplace.
“All of our tried and proven communications and outreach strategies that have worked well for other populations that we serve, they don’t work for this population,” Kofman told The 51st.
Hernandez, an Alliance member for over two decades, wants local leaders to recognize the impact of their decisions.
“We really need their help,” Hernandez said. “Not only for my family — I am asking for everybody, equally, because we need the insurance for our health.”
Gabby Salado, a student services coordinator at Briya Public Charter School, has witnessed the impacts of cuts on low-income immigrants firsthand.
She recalled one instance where a student in her adult education classes didn’t show up to class for a few days and then missed an appointment to help him navigate social services. Salado gave him a call, and learned that he hadn’t been coming because his face was swollen and his teeth were causing him too much pain.
“The obvious question was, like, ‘Well, have you gone to the doctor?’” Salado recalled. “His answer was simply, ‘No. I have no money. This is too expensive for me.”
The Ward 1 resident ended up in the emergency room that night, Salado said. He and his wife texted her from the hospital with questions about how to navigate billing.
Salado says he’s a former Alliance member, among the roughly 8,600 people who have lost their coverage since DHCF lowered the program’s income limit in October — a steep drop from 27,600 to 19,000 beneficiaries as of the first quarter of this year. Deputy Mayor for D.C. Health and Human Services Wayne Turnage has attributed the decline to tighter eligibility requirements, a moratorium on new enrollments, and also a fear of immigration enforcement.
Because of their immigration status, the overwhelming majority of these former beneficiaries aren’t eligible for any other publicly funded healthcare programs. Among roughly 2,200 people who lost coverage at the end of September, for instance, only 55 were identified as potentially eligible for Healthy DC or a Qualified Health Plan.
Before October, Salado said her office often helped students apply to Alliance, but the program now no longer accepts most new enrollees over age 25. Instead, a more stringent income cap at 138% of the federal poverty level — about $22,000 per year, for a one-person household — has brought painful decisions to many families still on Alliance.
“A lot of the families were like, ‘We barely make enough to pay rent, but now they’re saying that we make too much for healthcare,’” Salado said.
Some beneficiaries now must walk a careful line, earning enough money to provide for their families, but not making so much that they lose their healthcare.
“They pass up the bit of extra income that they could get, out of fear to lose their benefits,” she said.
People who lost Alliance coverage — such as Salado’s student who ended up in the ER — find themselves in an even more precarious position. For instance, Hernandez’s husband, who is the sole breadwinner for their household of four, has been left paying $435 every few months to cover his blood pressure medicine, and can no longer afford another medication that he takes for his diabetes, which would cost $1,000 for a refill, Hernandez said.
Some former beneficiaries have been finding help at federally qualified health centers like Mary's Center and La Clínica del Pueblo, which offer care on a sliding pay scale and are obligated to help people regardless of their insurance status. Even so, tight finances and limited awareness about available options have left many families weighing the cost of taking care of their health against other needs like paying rent and buying food.
“If the medicine is cheap, [families] cover it. If the medicine is expensive, they don’t,” Hernandez said.
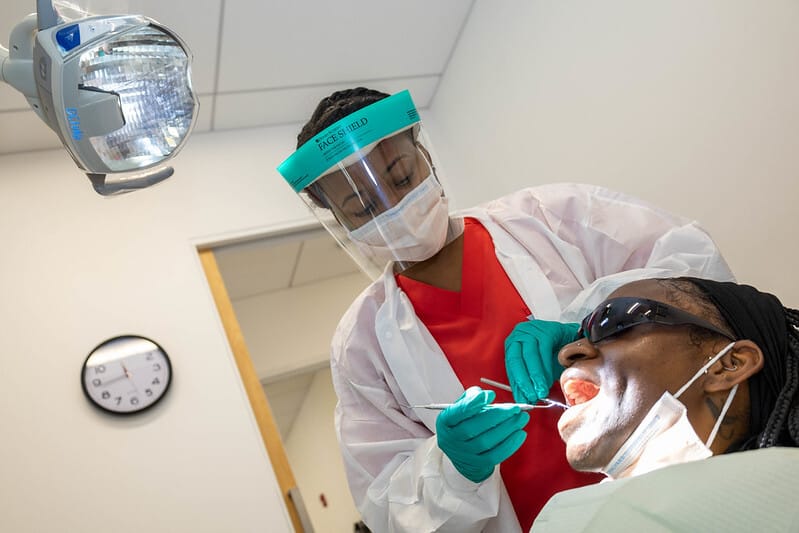
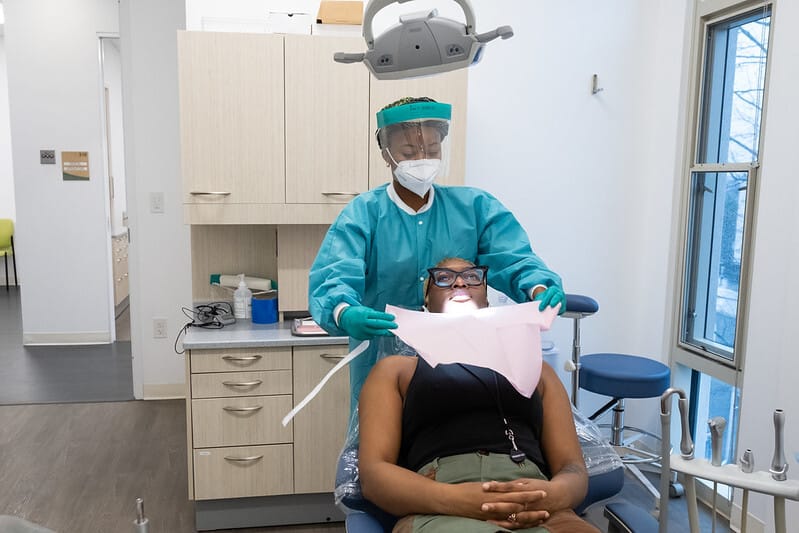
Patients at Bread for the City's dental clinic, which has been treating some of those who lost Alliance coverage.
When around 17,000 D.C. residents lost Medicaid coverage in January, it triggered weeks of confusion for some of D.C.’s most vulnerable patients.
Faith, a social worker at a D.C. cancer center who asked to go by her middle name because she isn’t authorized to speak to the media, said the change brought immediate chaos to her workplace as patients began showing up with Medicaid cards that no longer worked. When administrators checked these patients’ insurance status, they were all listed as uninsured.
“It was just, like, two full weeks of total pandemonium, and we received basically no guidance from the D.C. government ahead of time about how to navigate these changes in coverage,” said Faith, who has since left that facility to work for a different cancer center in Virginia.
The Health Benefit Exchange had mailed new member ID cards and multiple notices to all 15,000 people who were automatically added to Healthy DC, and had coordinated with groups like the DC Medical Society and DC Hospital Association on informing physicians. However, Kofman said that information about how to access new ID numbers may not have reached office managers or front office staff, and that many beneficiaries didn't realize the significance of the mail they received.
Additionally, Kofman said her team has been successful in contacting only about 300 of the 2,200 people who lost Medicaid and are ineligible for Healthy DC, despite multiple rounds of calls, texts, emails, and notices.
“You make things seamless, and run the risk that some patients will not know that things have changed,” Kofman said.
While Faith’s team eventually sorted out the logistics, complications have continued for patients who used to rely on Medicaid to get rides to appointments. Healthy DC doesn’t cover non-emergency transportation, presenting a problem for patients who don’t have a car, can’t afford a rideshare and, in some cases, are too sick or immunocompromised to take transit.
Gwen Umbach, a paralegal at another D.C. healthcare facility, described one instance of a patient calling the fire department for help because ice and snow prevented her from getting to a bus stop. In the past, Medicaid would have covered a ride directly from her doorstep.
Some patients with disabilities are still able to get rides through the MetroAccess Paratransit program for a couple dollars. Even so, Umbach said the cost and the extra effort create new barriers.
“I have one patient who has rescheduled a meeting with me three or four times now, because she doesn’t have a friend or family member available who can drive her … and she doesn’t have the money for any other option,” she said.
DHCF did not respond to questions about how many Medicaid members use non-emergency transportation each year, or how much it would cost to restore Healthy DC members’ access to this benefit.
More issues may be coming down the pipe for Healthy DC beneficiaries because the program also doesn’t cover vision or dental insurance. Dr. Steven Myles, the senior dentist at Bread for the City, has already been witnessing health impacts on members of Alliance since that program stopped covering dental in October.
While Bread for the City provides patients with full-service care whether they have insurance or not, the health center sometimes has to refer patients to specialists for more complicated procedures. But that’s not a viable option for low-income people without dental insurance, who may end up having to choose between living with pain and losing a tooth.
“We’re seeing a lot more extractions, or people just losing their teeth when they could have saved their teeth,” Myles said.
In addition to patients losing their dental insurance, Myles noted that fear from the increase in deportations may be making some people afraid to seek care.
Major decisions about the future of D.C.’s healthcare programs are at stake during this year’s budget season — and storm clouds are already gathering. While several councilmembers have joined a push to restore benefits to Alliance and Healthy DC members, Bowser has expressed commitment to keeping current reductions in place and moving forward with plans to end adult enrollment on Alliance by October 2027.
One pressure point concerns $21 million that the D.C. Council approved to restore current Alliance members’ benefits. While CFO Glen Lee greenlit DHCF to spend this funding in December, the agency hasn’t done so yet.
Bowser voiced concerns at the February breakfast meeting about “whiplash” if Alliance members see benefits temporarily restored, but then taken away again this October, when DHCF is on track to reduce the program’s income limit once again.
“We made some very well informed, difficult decisions last year around this, and they’re turning out pretty well in terms of how these programs are operating, so I would invite you to stick with them,” Bowser said.
Her stance prompted criticism from policymakers including Ward 5 Councilmember Zachary Parker, who noted that the $21 million is in the budget that the D.C. Council approved and that has been signed into law.
It remains unclear when, if ever, Bowser and the Council will reach an agreement on how to spend the money. Neither DHCF nor At-Large Councilmember Christina Henderson, chair of the Council's Committee on Health, responded to inquiries.
In the meantime, four councilmembers have signed a letter urging Bowser to restore funding for various social programs in this year’s budget proposal — returning Alliance to previous eligibility levels and adding benefits including dental and vision coverage for Healthy DC members, among other changes.
“The safety net is at risk of being dismantled and in desperate need of corrective action,” wrote Henderson, Ward 1’s Brianne Nadeau, Ward 4’s Janeese Lewis George and Ward 6’s Charles Allen.
Bowser, by contrast, pointed to healthcare costs that are rising faster than inflation and $700 million less available revenue projected in the coming fiscal year. In financial times like these, she argued, some forms of support for D.C.’s most vulnerable residents are just too expensive.
“I believe that the current changes put us on a more sustainable path, and that’s likely what I would advance again,” Bowser said.
With your help, we pursue stories that hold leaders to account, demystify opaque city and civic processes, and celebrate the idiosyncrasies that make us proud to call D.C. home. Put simply, our mission is to make it easier — and more fun — to live in the District. Our members help keep local news free and independent for all: